|
Islet Transplantation 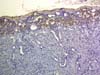

Experimental islet transplantation
started more than 3 decades ago with the discovery that islets of Langerhans
could be separated from the pancreatic tissue with collagenase. Islet
allotransplantation could potentially replace pancreas transplantation for the
treatment of Type 1 diabetics. Islet autotransplantation can be used to prevent
diabetes mellitus following a major pancreatectomy. As of today 400-500 islet
allotransplantations and 200-300 autotransplantations have been performed
worldwide. The success of islet transplantation in humans is limited, with no more than 20% of patients achieving complete normalization of glucose metabolism. The long-term function of transplanted islets has been poor with most grafts showing deterioration in function within 5 years. The main obstacles to successful islet transplantation
are: a) relatively small beta
cell mass available after islet purification, b) autoimmune and alloimmune
islet cell destruction, c) current use of diabetogenic immunosuppressants. The main mode of islet
transplantation consists of intraportal embolization. Other potential sites for transplantation include the spleen and
the kidney capsule. The morphological
aspects of allo- and autoimmune islet graft destruction are well known through
experimental studies. These consist of lymphocytic isletitis and eventual
disappearance of the hormone producing cells. In clinical practice tissue
evaluation is not used for the diagnosis of islet rejection. In experimental studies sophisticated
methods for the detection of islet rejection have included the demonstration in
serum of elevated levels of endogenous islet proteins and daily sequential
intravenous glucose tolerance tests. In addition to islet transplantation, other strategies
for treatment of type I diabetes are being
investigated. These include fetal
pancreas transplants, genetically engineered beta-cell lines and gene therapy,
implanted insulin pumps and artificial pancreas units. Xenotransplantation
(i.e. porcine islets) or in vitro expansion of cultured beta-cells could in
theory represent the solution for the problem of limited
pool of islet tissue for transplantation.
References
Please mail comments, corrections or suggestions to the TPIS administration at the UPMC.
If you have more questions, you can always email TPIS Administration. |
|