|
Post-Transplant Needle Biopsies Workup for allograft dysfunction: The major cause of graft loss with pancreas transplants is irreversible rejection. This is particularly true for pancreas after kidney (PAK) and pancreas transplant alone (PTA) cases since the clinical diagnosis of rejection remains relatively non-specific. When a simultaneous kidney transplant (SPK) is performed in an uremic diabetic the co-transplanted kidney is thought to provide a reliable indicator for rejection through serial determinations of the recipient's serum creatinine. Parameters used for the diagnosis of pancreas rejection include: decrease in urinary insulin and C peptide, increase in serum amylase, lipase, anodal trypsinogen and pancreas specific protein). Cytologic evaluation of pancreatic juice and urine have been also used in the diagnosis of pancreas allograft rejection. In bladder drained grafts, urinary amylase has been used as a measure of pancreas exocrine function. Other methods used for the diagnosis of pancreas rejection are 99mTc DTPA scintigraphy and uptake of indium-labeled platelets. The success of renal, hepatic and cardiac transplantation, has been dependent on the ability to differentiate non-immunologic causes for graft dysfunction from rejection by reliance on a confirmatory biopsy. Biopsy material from transplanted pancreas was obtained in the past during laparotomy or through cystoscopically guided transduodenal pancreatic biopsy. The use of percutaneous pancreas graft biopsies has has yielded tissue for histologic analysis in greater than 88% of attempts, with complications in fewer than 2% of cases. The biopsies are performed under ultrasound guidance using an 18-gauge automated biopsy needle with a 17mm specimen notch. The material is routinely fixed an processed. Twelve 4 micron sections are cut and levels 1,4,8 and 11 are stained with H&E. The remaining slides are used for additional stains if necessary (CMV, lymphoid markers, EBER, LMP-1, etc.) Or stored. The average surface area of each tissue section is 2mm3. Two to three segments of parenchymal lobules with corresponding fibrous septa are suitable for evaluation.
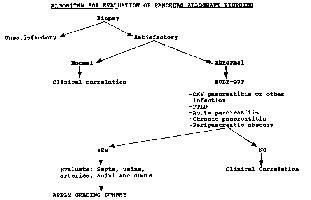
Protocol biopsies (normal pancreas, Grade 0): Pancreas needle biopsies from patients with normal graft function typically show no inflammation. The reticulin stain highlights a delicate reticulin network outlining the acini and islets. Sometimes the tissue core includes parts of the peripancreatic fibrous tissue and skeletal muscle. In early post-transplant biopsies fat necrosis of the peripancreatic fat is common. The peripancreatic fibrous tissues often show foreign body giant cell reaction. Occasional biopsies contain fragments of benign lymph nodes. Biopsies from patients with normal function may also show inflammation of undetermined significance (Grade I). REFERENCES

Please mail comments, corrections or suggestions to the TPIS administration at the UPMC.
If you have more questions, you can always email TPIS Administration. |
|