|
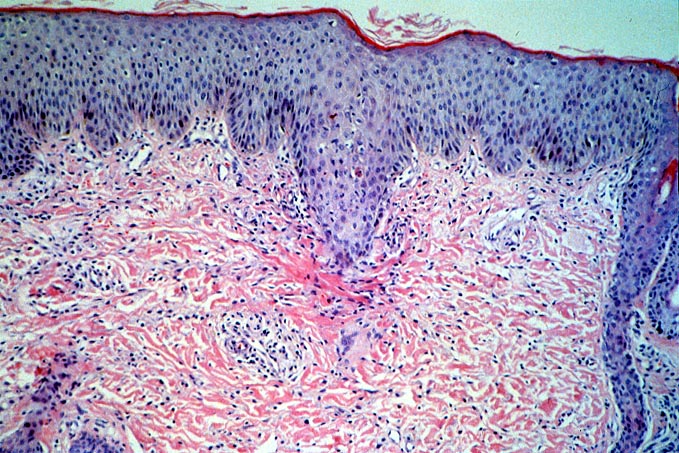
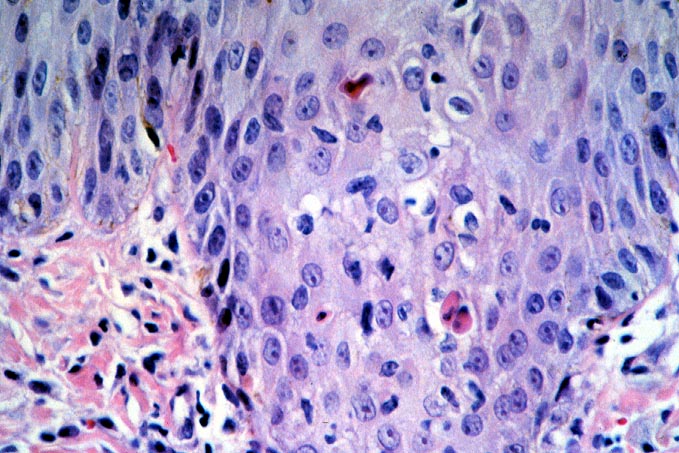
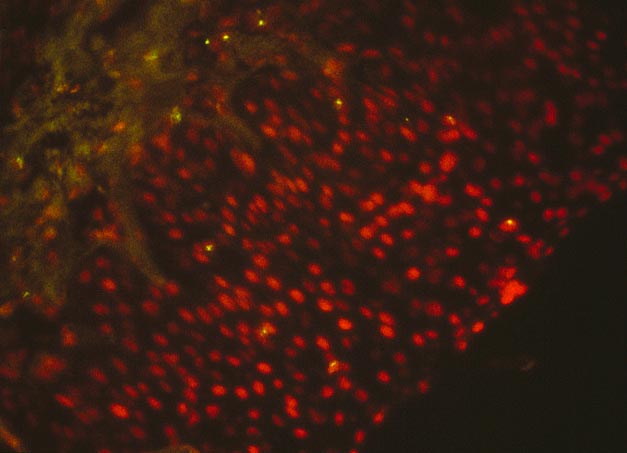
Graft versus Host Disease Because small intestine is rich in lymphoid tissue, it is not surprising to see that the incidence of GVHD in small bowel transplant patients is higher than in other solid organ transplantation. GVHD occurs in approximately 5% of patients receiving small bowel transplantation(1-2), which is approximately 5-10 times higher than in other solid organ transplantatiion. Most patients present with skin rash. Other clinical presentations include ulceration of oral mucosa, diarrhea, or native liver dysfunction. Onset of clinical symptoms occurred from 8 days to several years postoperatively. The diagnosis is usually established by histopathological criteria which include keratinocyte necrosis, epithelial apoptosis of the native gastrointestinal tract or oral mucosa. Donor cell infiltration can be demonstrated by immunohistochemical methods. The histological features and diagnosis criteria are similar to those in the classical GVHD after allogenic bone marrow transplantation. GVHD occurred in most of the small bowel allograft recipients is usually not fatal by itself because of the heavy immunosuppressive therapy, though opportunistic infections secondary to the heavy immunosuppression are the frequent cause of death in these patients. The morphological features of intestinal GVHD and acute rejection share a great degree of similarity. Both conditions histologically manifest with crypt cell apoptosis and pathogenetically show increased expression of TNF-a and involvement of cytotoxic T lymphocytes. The morphological similarities are most striking with latter instances of acute rejection in which apoptosis tends to be more pronounced and cellular infiltration is often less severe. In the latter episodes of acute rejection, the allograft gut-associated lymphoid tissue has been replaced by recipient lymphoid cells and immune reactivity is directed primarily at epithelial and stromal cells. Therefore, the overall immunologic process in latter episodes of acute rejection are more akin to GVHD. Obviously, because of the morphological similarities between acute rejection and GVHD, histological diagnosis of intestinal GVHD can only be made in the biopsies obtained from the native intestine. REFERENCES 1. Abu-Elmagd K, Reyes J, Todo S, Rao A, Lee R, Irish W, Furukawa H, Bueno J, McMichael J, Fawzy AT, Murase N, Demetris J, Rakela J, Fung JJ, Starzl TE. Clinical intestinal transplantation: New Perspectives and immunologic considerations. J Am Coll Surg 1998; 186:512-527. 2. Mazariegos, G. V., Abu-Elmagd, K., Jaffe, R., Bond, G., Sindhi, R., Martin, L., Macedo, C., Peters, J., Girnita, A., and Reyes, J. Graft versus host disease in intestinal transplantation. Am J Transplant, 4: 1459-1465, 2004.
Please mail comments, corrections or suggestions to the TPIS administration at the UPMC.
If you have questions, please email TPIS Administration. |
||||