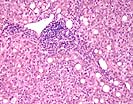
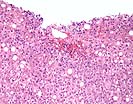
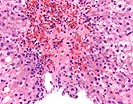
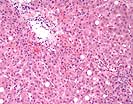
In this series of biopsies there are qualitatively similar changes throughout, but quantitatively there are some variations in the sequential samples. Therefore, the sequence will be described together with particular reference to each sample and then an overall impression will be given on the patient course and in particular on the most recent biopsy.
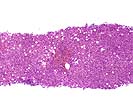
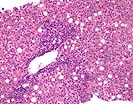
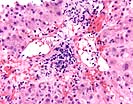
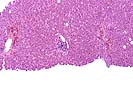
In the first two samples, Part A & B, there are two constellations of histopathological findings. The first is a severe central venulitis characterized by lymphoplasmacytic perivenular inflammation associated with variable degrees of congestion, hepatocyte dropout, and deposition of pigmented macrophages and variable central vein fibrosis. This constellation of findings is interpreted as an ongoing cellular rejection with severe central venulitis. In addition, both biopsies show mild spotty acidophilic necrosis of hepatocytes, a mild to moderate portal inflammatory cell infiltrate with focal interface activity as well as a Type 2 ductular reaction, combined with variable lymphohistiocytic lobular inflammation, lobular necro-inflammatory activity and macrovesicular steatosis. This constellation of findings is interpreted as a background of active hepatitis, most likely attributed to recurrence of the chronic hepatitis C virus infection.
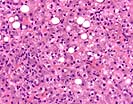
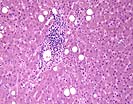
In the third biopsy, Part C, both sets of findings persist, but the central venulitis is particularly noticable, which now would be diagnosed as at least a mild acute cellular rejection with a background of recurrent viral hepatitis C.
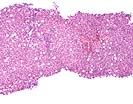
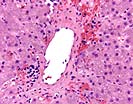
In the most recent sample, Part D, the overall histologic appearance of the biopsy is improved compared to the previous samples: there is less portal and perivenular infiltration. However, there is ongoing persistent central venulitis with focal perivenular fibrosis. In addition, there is spotty acidophilic necrosis of hepatocytes without much lobular inflammation. This spotty necrosis is likely attributable to the recurrent hepatitis C virus infection but cytomegalovirus should be excluded.
Overall, it is my opinion that the ongoing central venulitis represents a component of acute rejection that persists throughout all of the samples, and is the predominant histopathological finding responsible for most of the liver allograft injury. While there are background changes of recurrent hepatitis C, it is my opinion that those have been secondary in importance. However, it is always difficult in such cases to determine which disorder requires therapeutic attention. If one aggressively treats the acute rejection, the hepatitis viral replication will likely increase and the hepatitis may worsen, with the risk of developing a cholestatic variant hepatitis. Conversely, lowering immunosuppression can worsen the rejection-related injury. In this particular patient, the persistence of the centrilobular inflammation and dropout, along with the development of focal perivenular fibrosis are the most worrisome findings at this time. It has been my experience, that some of these patients will go on to develop ascites and significant problems from the perivenular fibrosis that can develop as a response to the central venulitis. Therefore, I would probably opt with treatment of the central venulitis with close monitoring for flare-up of the hepatitis. Lastly, as central venulitis can be seen more commonly with autoimmune hepatitis, an overlap of autoimmune hepatitis, or autoimmune hepatitis precipitated by C virus should be excluded. I look forward to any follow-up in this difficult case.