Previous Biopsies on this Patient:
None
TPIS Related Resources:
Liver Transplant Topics
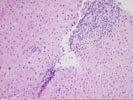
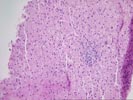
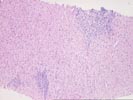
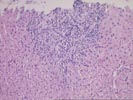
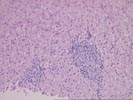
Part 1 The specimen consists of a small fragmented needle core biopsy of liver with an intact, but slightly distorted lobular architecture. The portal tracts are mildly expanded because of a mild mixed inflammatory cell inflammatory cell infiltrate and mild duct and cholangiolar reactivity. In one portal triad, the mononuclear infiltrate focally impinges on the ductal epithelium, which shows reactive stratification and slight papillary enfolding. Focal destruction of the ductal basement membrane is also seen in one duct. Mild interface activity is also present.
Throughout the lobules, there is mild disarray, Kupffer cell hypertrophy, thickening of the plates and mild lymphohistiocytic lobular inflammation. However, no definite ground glass cells nor viral inclusions nor prominent pigment deposition is seen. An occasional small Kupffer cell granuloma is appreciated.
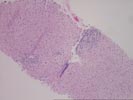
Part 2 Compared to the previous biopsy, the portal inflammation and expansion have increased, mostly because of mild to focally moderate fibrosis and a ductular reaction at the interface zone.
On closer examination, the triads contain a predominantly mononuclear but mixed inflammatory cell infiltrate. Small bile ducts are difficult to locate. A few seen show reactive changes. There is moderate spillover of the inflammation into the edge of lobules with ongoing interface activity. One duct shows evidence of lymphocytic cholangitis.
Some lysosomal pigment deposition is present in periportal hepatocytes.
Throughout the lobules there is thickening of the plates, mild Kupffer cell hypertrophy, occasional small Kupffer cell granulomas and mild lymphohistiocytic lobular inflammation. However, no prominent pigment deposition, nor ground glass cells nor viral inclusions are seen.
Overall, the focally severe bile duct damage in the first biopsy; the papillary enfolding of the biliary epithelium; the progressive portal expansion noted in the second biopsy with the ductular reaction and periportal lysosomal pigment deposition are suggestive of a "biliary" etiology. This is consistent with the preferential elevation of the gamma glutamyl transpeptidase and alkaline phosphatase noted on recent liver injury tests.
Considering the age and sex of the patient and the histopathologic findings our leading consideration would be primary biliary cirrhosis/autoimmune cholangitis, contingent upon evaluation of the anti-mitochondrial antibodies. Other, less likely possibilities include an adverse drug reaction; and mechanical causes of biliary tract obstruction or stricturing. I look forward to any follow-up in this case.