Previous Biopsies on this Patient:
None
TPIS Related Resources:
National Cancer Institute PDQ treatment information on liver cancer
Liver Transplant Topics
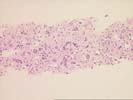
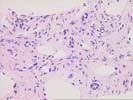
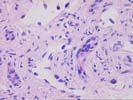
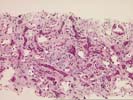
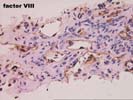
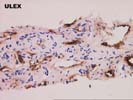
The sections comprise one needle core consisting of thin-walled vascular channels with rounded and irregular profiles within a loose fibrous stroma that contains proliferated ductules, occasional arteries, and associated scattered neutrophils. These vascular channels are lined by occasionally plump and focally hyperchromatic cells that are demonstrated to be endothelial in nature by factor VIII and Ulex immunostains. No solid nests, foci of necrosis, or mitoses are identified. Additional needle cores show relatively normal liver parenchyma with focal congestion and sinusoidal dilatation. The portal tracts are largely unremarkable. Scattered in the sinusoids are occasional large sinusoidal lining cells that prove to be Ulex and factor VIII positive.
The mass seen here does not conform well to any of the standard liver neoplasms. The lesion appears to be vascular in nature and not typical of focal nodular hyperplasia, hepatocellular adenoma, or mesenchymal hamartoma. Features that are unusual for the typical hemangioma of the liver include the size and hyperchromasia of occasional nuclei lining the vascular spaces, and the finding of similar nuclei within the adjacent normal liver, suggesting some degree of local invasion. We are unable to make an outright diagnosis of angiosarcoma, but the atypical features raise the possibility of a low-grade malignancy. Consequently the lesion should be resected, if at all possible. This case was also reviewed by Drs Nalesnik and Demetris, who agree with the diagnosis.
Thank you for sending this fascinating case and we would appreciate follow-up information as it becomes available.